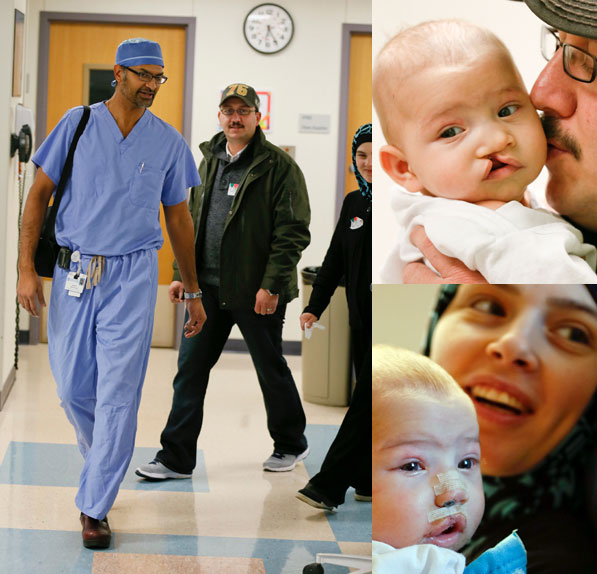
At left, Dr. Murthy brings Noor’s parents back to see her in the recovery unit after the first surgery for the lip and nasal correction. Top right and bottom right is Noor before and after the lip and nasal surgery in December 2013.
April 9, 2014 Dr. Ananth Murthy performed a cleft palate surgery on Noor Mustafa. Dr. Murthy explains the surgery’s 8 major steps, how the OR is staffed, and talks about the expectations, follow-ups, the outlook and speech development issues associated with cleft palates. You can read or listen to Dr. Murthy below.
Introduction
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/overview.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
Hi. I’m Dr. Ananth Murthy. I’m a pediatric plastic surgeon at Akron Children’s.
This is Noor Mustafa. She’s now 8 months old and ready for her palate correction. When she was much younger she had an appliance placed in her mouth which helped line up her gum line and lips. We performed the lip correction when she was close to 3 months old. She has now healed very well from her lip and nasal correction and now presents for closure of her palate. See Noor’s previous surgery in this blog post.
Outlook
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/outlook.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
Typically the operation takes a couple hours. After surgery the child is taken to the recovery room where they’re observed for maybe 45 minutes to 1 hour to make sure they woke up well and are behaving normally.
After that we send them up to the floor where we watch all the children who have undergone surgery. Typically a child who has a cleft palate spends about 24 hours in the hospital. They stay overnight and the next morning we remove the gauze packing from the roof of the mouth. After they’re feeding well, they can go home. That process takes about 24 hours.
Following up after the surgery
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/follow-up.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
After the child is discharged from the hospital, we typically see them at 1 week after surgery and 3 weeks after surgery to make sure there are no surgical complications. I then recommend that they follow up with us when they are about 1 year of age in our multidisciplinary craniofacial clinic so that we can correctly assess their speech and hearing, appearance of the lip and function of the palate.
Expectations
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/expectations.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
Typically one of the first things that parents tell me after such an operation is that the child no longer has any food coming out of their nose when he/she eats.
For the first 3 weeks after surgery we have them on a liquid or pureed diet which is not a problem at this age. Parents are usually very happy that nothing is coming out of their nose at that point.
After a few months, when the little babies get used to the new orientation of the muscles of their soft palate, they are even able to transition out of the modified cleft models to regular or sippy cups.
Below, Dr. Murthy covers the major points during this surgery:
Step 1:
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/1.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
The first step will be to make incisions. Typically these incisions are along the back, or the posterior portion of the gum line, and then extend along the edge of the cleft all the way to the back where the uvula hangs.
Step 2:
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/2.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
Then I’m able to raise the layer of tissue that’s on the oral surface of the hard palate. This is raised right off of the bone of the hard palate. We’re careful to see that the blood vessel that supplies nutrition to this portion of the palate is intact. This dissection is also carried into the soft palate to expose some of the muscles.
Step 3:
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/3.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
Using an elevator, I’m able to raise the oral mucosa or the oral layer that covers the soft palate away from its underlying muscles. It’s important for me to dissect this so that I can visualize all the muscles in the soft palate in order to repair them correctly.
Step 4:
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/4.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
In terms of speech — the most important muscle of our soft palate is the levator veli palatini. This muscle helps pull the soft palate up, or elevate it, so that it can close against the back of the throat or the pharynx. It’s important to me that not only do we find the muscle, but also try to push it back as far as possible, so that when the muscle does contract we’re able to achieve the closure that’s necessary for normal speech.
Step 5:
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/5.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
After all the muscles have been dissected and tagged, the first step is to close the nasal layer of the palate. I start near the hard palate and repair the nasal layer and take it all the way back to the uvula. I perform an operation where a “Z” type incision is present in both the nasal and oral layers of the closure and I pay close attention to this while I’m performing the closure of the nasal layer.
Step 6:
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/6.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
We then proceed to repair the uvula. The uvula is that little piece of tissue that hangs in the back of the palate. That’s what we all remember seeing when we look at the soft palate. I believe that it’s important to repair this correctly even though it doesn’t have a functional aspect to it. It kind of tells you that whoever did the palate repair did a good job if that uvula’s together.
Step 7:
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/7.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
I then repair the muscles of the soft palate. As I mentioned earlier, we had already dissected and tagged the levator muscle. Now I repair them end-to-end and then progressively tighten this muscle repair with a few more sutures. This allows me to not only push the muscle farther back, but also achieve good tightening across the muscle repair. I’m hoping with this amount of tension on the muscle, that as it contracts, it can close that gap behind the soft palate easily.
Step 8:
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/8.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
After we repair the muscle all that’s left to do is close the oral layer of the palate. We start at the soft portion of the palate and progress towards the hard portion of the palate and repair both edges of the cleft to one another.
Speech Development
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/8.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
In spite of all our best efforts, this type of an operation is only about 80 to 90 percent successful depending on how bad the cleft is.
Typically children start to babble and experiment with oral sounds around 7 to 8 months of age. They develop some of their first words around 1 year of age where they’re able to use it purposefully.
I try to repair the palate before that time to allow for the best chance to develop normal speech and to not have any compensatory problems because of a lack of a closed cleft palate.
Around 18 months of age we evaluate them to see where they are with their speech and language development.
Around 3 to 4 years of age we’re able to tell if this operation is successful or not.
Like I said — there is that percentage of patients who are not successful after this operation — they continue to have nasal sounding speech (hyper resident speech). In that case they will need some diagnostic tests and quite possibly surgical correction to decrease that air loss through their nose.
We don’t typically explore that until they’re about 3 to 4 years of age.
Dr. Ananth Murthy explains how the operating room is staffed for the cleft palate operation on Noor. Listen to Dr. Murthy below or read the transcript.
[ca_audio url_mp3=”https://inside.akronchildrens.org/wp-content/uploads/2014/04/staffing.mp3″ url_ogg=”” height=”25″ download=”true” html5=”true” skin=”regular” align=”center”]
Q: Starting with you – who’s all in the room and what are they doing?
Dr. Murthy: Broadly it can be divided into 3 teams: the anesthesia team, the surgical team and the nursing team.
The nursing team is comprised of registered nurses as well surgical techs who assist in the operation. (They assist) with anything from getting the necessary equipment from outside the operating room to handing them to me directly to preparing the patient, helping with the IVs, waking them up and moving them. They take care of everything.
The anesthesia team is comprised mostly of the anesthesiologist and a mid-level provider such as a nurse anesthetist. Sometimes they may have an assistant in there or a student as well. They’re in charge of keeping the patient asleep and keeping them stable through the whole operation depending on what goes on in the operating room.
Q: How many people are on the nursing team?
Dr. Murthy: Typically 2 to 3 and it’s the same with the anesthesia team – 2 to 3.
The surgical team is myself and then I’ll either have my assistant, a resident and possibly a fellow so it could be anywhere from 3 to 4 people as well.
Q: Is this assistant always the same person?
Dr. Murthy: For the video’s purposes it’s probably going to be the same person. I have a PA, her name is Candace. She’ll be in there or it could be the resident.
We have a very good residency program here in Akron where we train future plastic surgeons. They rotate through different hospitals and different services. Usually they spend a couple of months a year with me involved in these operations so they can learn to do it if they want to in the future.
Q: What might the assistant be doing during the operation?
Dr. Murthy: The assistant mostly sucks the blood, cuts sutures and retracts tissue away so I can find what I need. Depending on the level of the resident, they get to actually do some of the closure or dissection of the muscle.
These guys are all very well trained. They’ve already done 5 years of general surgery. They’re in their 6th, 7th, 8th years of training and I would trust them with my own children. I always reassure the families that anybody who’s going to be operating on their child — I would let them operate on my own child. That usually makes them feel better about having that surgical assistant in the room.
Q: What’s the hierarchy in the operating room?
Dr. Murthy: It’s not like a hierarchy. It’s a much different dynamic and it’s not like basketball either. We’re all doing stuff, but the only person doing something to the patient is the surgeon. I’m the guy cutting, but I need everybody else to allow me to do that so the dynamic is different.
It’s not like Formula One racing where you have one driver in the car but you need the engineers, the pit crew, the owners and everybody else to help. It’s not that because there’s more to it.
It’s almost like flying an airplane maybe. That’s probably the closest. You have the tower, the crew, the staff on the planes, the pilot and the engineers. I would say it’s very similar to that.
Actually the surgical world has really embraced that mentality of flying a plane because the airplane industry has some of the best safety standards of any industry. The medical field needs to be there.
We have adopted things they have used before like the checklist where you go over your plan and you confirm it with your staff and the tower and you do the same thing in surgery now.
I think it’s something to look up to as far as safety in a particular industry.









